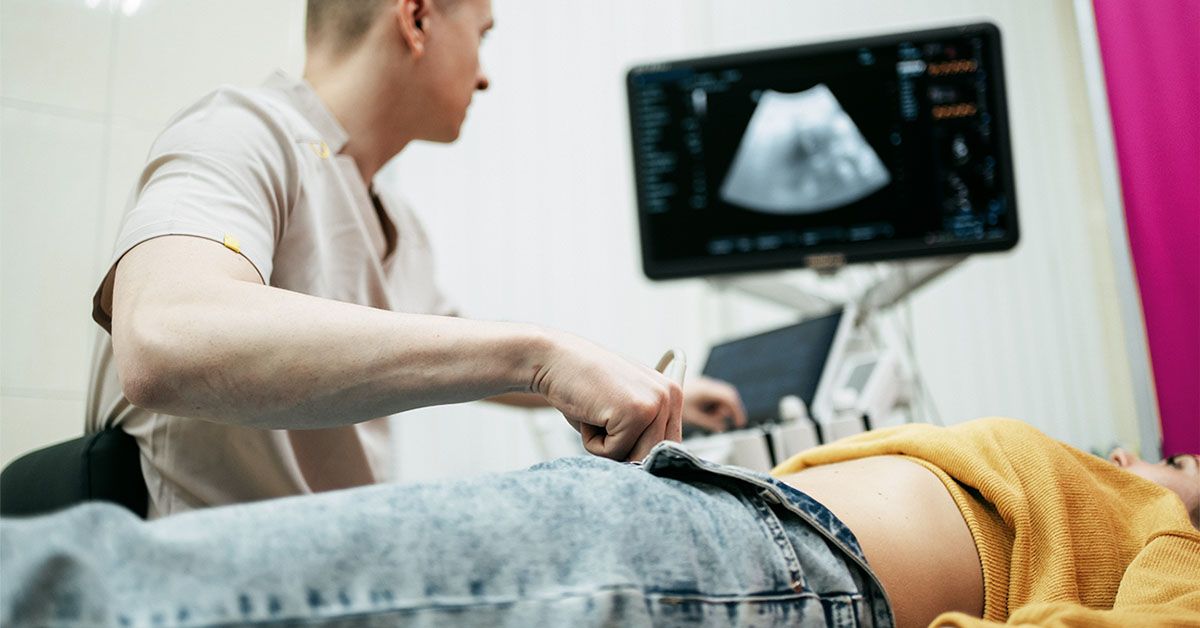
- New pointers from the American Most cancers Society endorse self-collection of vaginal specimens for HPV testing in medical settings.
- Females should be between 25 and 65 and have a median threat to be eligible for self-collection.
- Adjustments have additionally been made within the exit standards for older females.
- Extra stringent most cancers screening is now required for females to stop testing.
- The objective is to enhance screening entry and scale back excessive most cancers charges over age 65.
The American Most cancers Society (ACS) has up to date its cervical most cancers screening pointers to endorse self-collected vaginal specimens for human papillomavirus (HPV) testing, marking a significant shift in U.S. screening practices.
The adjustments permit average-risk people ages 25 to 65 to gather their very own samples in medical settings — or, in restricted instances, at residence — utilizing FDA-approved kits.
The replace goals to enhance screening entry and fairness by eradicating boundaries for underserved populations, whereas additionally revising exit standards to require HPV testing at ages 60 and 65 to handle persistently excessive most cancers charges in folks over 65.
This follows latest Meals and Drug Administration (FDA) approvals of a number of HPV assessments and assortment units to be used in medical settings, in addition to one possibility for at-home assortment.
Traditionally, cervical cancer screening relied on clinician-collected samples obtained throughout a pelvic examination, both for a Pap smear alone, HPV testing, or a mixture of each.
Whereas efficient, this method generally is a barrier for many who face discomfort, restricted entry to care, or different obstacles to in-person screening.
HPV testing utilizing self-collected vaginal specimens has now been proven to have sensitivity and specificity akin to clinician-collected samples when PCR-based assays are used.
A number of research and meta-analyses reviewed by the ACS Guideline Growth Group (GDG) discovered excessive settlement between the 2 strategies, significantly for detecting excessive threat HPV sorts linked to cervical precancer.
Beneath the brand new ACS steering, average-risk people could self-collect vaginal specimens for HPV testing utilizing FDA-approved kits. These broadly out there kits are at present designed to be used inside healthcare settings underneath the steering of a primary care physician or gynecologist, in keeping with the ACS pointers.
The one FDA-approved possibility for at-home self-collection is at present the Teal Wand, which has restricted availability and is barely supplied by way of a proprietary telehealth service.
If the result’s destructive, repeat screening is suggested in three years, which is a shorter interval than the 5 years beneficial for clinician-collected HPV assessments. The ACS refers to this as a “margin of security” whereas awaiting extra long-term U.S. information on self-collection efficiency.
Authorised choices embrace:
- Roche cobas HPV take a look at with FLOQSwab or Evalyn Brush
- BD Onclarity HPV take a look at with FLOQSwab
- Abbott Alinity m with Evalyn Brush or Qvintip swab
- Teal Wand for at-home use with the Roche cobas HPV take a look at (by way of a proprietary telehealth service)
Self-collection can’t substitute clinician assortment for sure higher-risk teams, nevertheless, corresponding to these with HIV, immunosuppression, prior cervical most cancers, or in utero publicity to diethylstilbestrol (DES).
These sufferers require each HPV and cytology testing, and cytology can’t be carried out on self-collected specimens.
The rule replace additionally addresses one other long-standing concern: unclear and hard-to-implement standards for exiting screening at age 65 and past.
About one-quarter of cervical cancers within the U.S. happen in females over 65, with mortality twice that of youthful females — an issue linked to insufficient screening within the years earlier than stopping.
Beforehand, the ACS suggested ending screening at age 65 if a person had a documented historical past of ample destructive assessments within the prior 10 years. In observe, this proved tough as a result of medical information had been usually incomplete, resulting in missed screenings.
The brand new suggestion takes a forward-looking method: average-risk people ought to have destructive major HPV assessments (most popular) or destructive co-tests at each ages 60 and 65 earlier than stopping screening.
If these usually are not out there, three consecutive destructive Pap assessments on the beneficial interval, with the final take a look at administered at age 65, are additionally acceptable. For these utilizing self-collected HPV testing, the three-year interval applies.
Screening ought to proceed previous age 65 for anybody with sure threat components, together with HIV, immunosuppression, irregular outcomes up to now 10 years, cervical precancer up to now 25 years, or any historical past of cervical most cancers.
By including self-collection as an evidence-based possibility and simplifying exit standards, the ACS goals to make cervical most cancers screening extra versatile, accessible, and efficient, whereas sustaining security by way of clear follow-up protocols and risk-based resolution making.
After this, screening may be completed each three to 5 years, relying on the take a look at used.
“Sufferers want to know that they now have the choice to gather their very own vaginal specimen for HPV testing at residence or in a medical setting,” Kahn informed Healthline, “however this requires extra frequent screening than conventional clinician-collected samples.”
Ryan added that whereas self-collection utilizing FDA-approved units and HPV assays is appropriate, clinician-collected cervical specimens are nonetheless most popular.
“Moreover, sufferers ought to know that the standards for stopping screening have modified — they now want destructive HPV assessments at each ages 60 and 65 years to securely exit screening, slightly than the earlier much less stringent necessities,” he mentioned.
Jennifer Lincoln, MD, an writer, ladies’s well being advocate, and board licensed OB-GYN, mentioned that the ACS’s updates signify progress in cervical most cancers screening, particularly on the subject of decreasing boundaries to care. Lincoln wasn’t concerned within the new pointers.
Talking concerning the allowance for self-collected samples for HPV testing, she mentioned, “That is vital as a result of over 1 in 4 U.S. females are behind on screening, with 32% citing discomfort as a barrier.”
Lincoln additional famous that a number of teams of females, together with these in rural areas, these with out simple healthcare entry, trauma survivors, and anybody who feels uncomfortable with speculum exams, can profit from these adjustments.
That is particularly noteworthy, she added, as a result of females in rural areas face larger cervical most cancers mortality.
“A number of testing choices additionally enhance the probability that sufferers will truly get screened by assembly them the place they’re,” mentioned Lincoln.